- Center on Health Equity & Access
- Clinical
- Health Care Cost
- Health Care Delivery
- Insurance
- Policy
- Technology
- Value-Based Care
Medicaid Expansion's Unfinished Map: Some Southern States Still at a Crossroads
Medicaid expansion significantly improves health coverage and access, yet several Southern states face a persistent coverage gap amid political challenges.
The map of Medicaid expansion across the US, as tracked by KFF's "Status of State Medicaid Expansion Decisions", continued to illustrate a persistent divide, particularly in Southern states, even as the Affordable Care Act (ACA) marked its 15th anniversary this year.1,2
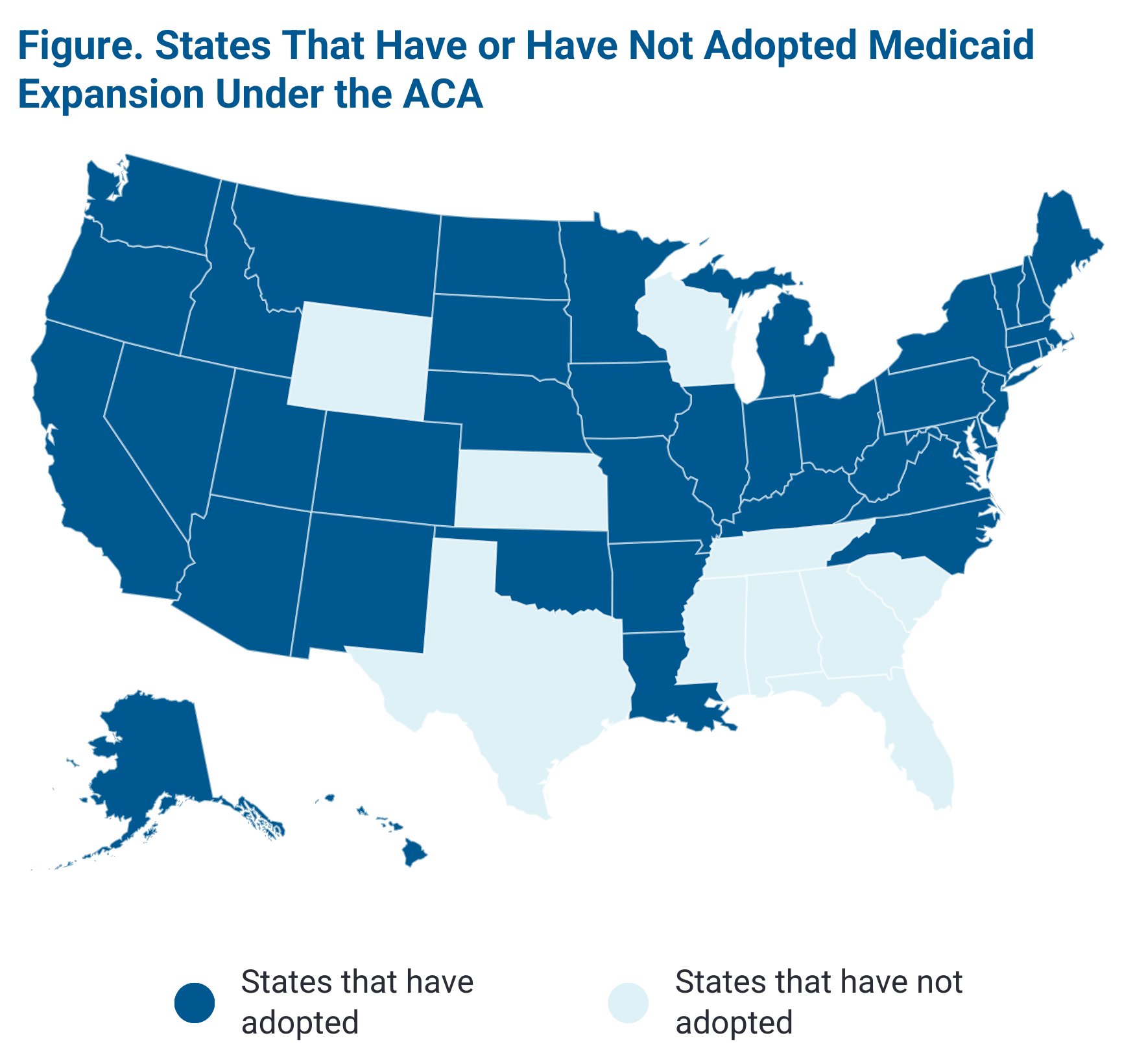
Originally, the ACA aimed to expand Medicaid coverage to nearly all adults with incomes up to 138% of the Federal Poverty Level (FPL) and offered states an enhanced federal matching rate ($21,597 for an individual in 2025).3 However, a 2012 Supreme Court ruling rendered this expansion optional for states. By early 2025, 41 states, including the District of Columbia, had adopted the Medicaid expansion, whereas 10 states had not (Figure).1
A critical area of focus remained on the Southern states, where a significant number of uninsured individuals fell into a "coverage gap".2 This gap existed in non-expansion states for adults with incomes above their state’s Medicaid eligibility but below the poverty level, rendering them ineligible for ACA Marketplace subsidies, which were not provided below poverty in anticipation of mandatory Medicaid expansion. An estimated 1.4 million uninsured individuals were in this coverage gap across the 10 non-expansion states. Nearly three-quarters of these individuals resided in just 3 Southern states: Texas (42%), Florida (19%), and Georgia (14%).4 Overall, 97% of those in the coverage gap lived in the South, where 7 of the 16 states had not adopted Medicaid expansion. Uninsured rates in non-expansion states were nearly twice as high (14.1%) compared with expansion states (7.6%).
10 states have not adopted Medicaid expansion under the ACA, including Texas, Kansas, Wyoming, Wisconsin, Tennessee, South Carolina, Georgia, Alabama, Florida, and Mississippi. | Data source: KFF
The Proven Benefits of Medicaid Expansion
Medicaid expansion had demonstrable positive impacts on health coverage, access to care, and economic stability. Nationally, the ACA, primarily through Medicaid expansion, reduced the uninsured rate from 17% in 2013 to 10% in 2016.5 During this period, 18.5 million people gained health insurance, with Medicaid expansion accounting for 10.9 million of these gains. In expansion states, the uninsured rate was more than halved, dropping from 15.3% to 7%. The ACA's broad reach eventually provided coverage for more than 31 million Americans.2
Expansion was linked to reduced rates of uninsurance, increased health care affordability, and improvements in access.6 Uninsured individuals often experienced greater difficulties accessing care and were less likely to receive preventive services or treatment for major health conditions and chronic diseases.3,4 Research consistently demonstrated positive health outcomes, including a significant 3.6% decrease in all-cause mortality, largely attributed to a reduction in health care-amenable mortality. Declines were observed in mortality related to specific conditions such as certain cancers, cardiovascular disease, and liver disease.6 Studies also noted decreased maternal mortality and infant mortality among Hispanics.2,6
Medicaid expansion also improved coverage and access for individuals with chronic conditions and disabilities.5 Studies indicated increased insurance coverage for cancer patients and survivors, leading to earlier-stage diagnoses.5,6 Adults and teenagers with diabetes saw increased coverage, and access improved for various other chronic conditions, including HIV screening.6 The expansion also offered increased coverage options for people with disabilities and improved mental health outcomes for their caregivers. Furthermore, it improved access to care and outcomes for substance use disorder and mental health, including increased prescriptions for medication-assisted treatment for opioid use disorder.
Economically, expansion yielded benefits for both states and health care providers.3,6 Expansion states experienced increased federal Medicaid spending and realized net state savings by offsetting costs in areas such as SUD treatment and traditional Medicaid programs.6 Conversely, states that did not expand passed up an estimated $43 billion in federal funds in 2018. Health care providers, particularly hospitals, observed improvements in their payer mix (fewer uninsured patients, more Medicaid-covered patients), decreased uncompensated care costs, increased revenue, improved operating margins (especially for rural and small hospitals), and a reduction in hospital closures. Research also suggested that expansion reduced disparities in coverage by income and/or education status, and for some racial groups.
Trump Administration's Policies and Potential Impact on Medicaid Expansion
The future of Medicaid expansion faced new uncertainties under the Trump administration's policy initiatives.2,7 The House of Representatives passed a budget resolution in February 2025 that proposed $880 billion in Medicaid cuts.8 A revised proposal aimed to reduce the budget deficit by $912 billion by 2034, potentially leaving 8.6 million fewer individuals insured. These proposed cuts raised concerns about shifting significant financial burdens to states, jeopardizing coverage for millions, especially rural and low-income populations, and negatively affecting pediatric health care.2,7 Hospitals, community health centers, and nursing homes were also projected to be impacted.7
Specific contentious proposals for Medicaid funding included:
- Stricter eligibility requirements
- Monthly work requirements for adults 19 to 64 years old (excluding pregnant women)
- Citizenship checks
- Tougher screenings for health care providers
- Cutting Medicaid funding to states that offer coverage to illegal US residents Prohibiting Medicaid from funding gender reassignment surgery for children.
CMS also retracted guidance on social services for Medicaid and Children’s Health Insurance Program (CHIP), which had affected interventions related to housing, medically necessary home improvements, and nutrition.
Beyond Medicaid funding, the Trump administration pursued broader ACA rollbacks. President Trump issued executive orders reversing several Biden-era health policies, including scaling back ACA enrollment expansions and halting drug pricing initiatives. Robert F. Kennedy Jr's confirmation as HHS Secretary faced scrutiny due to his lack of a clear plan for Medicare and Medicaid and an "unclear grasp" of the distinctions between these programs. Although he criticized Medicaid's inefficiencies, he did not propose major cuts. Additionally, a Trump administration freeze on federal financial assistance initially raised concerns about its impact on Medicaid funding, leaving states uncertain about federal matching funds, though it was later blocked by federal judges.
Another significant challenge to the ACA’s preventive services mandate stemmed from the Supreme Court case Kennedy v Braidwood Management.9 This case questioned the authority of the US Preventive Services Task Force to recommend services insurers must cover without Senate appointment. A decision in favor of Braidwood could result in insurers dropping coverage for more than 30 key preventive services, including those related to HIV, cancer, and mental health care. The Trump administration's brief in the case, although aligning with previous arguments regarding oversight, could influence the outcome of service coverage mandates. Other health-related cuts considered by the administration included the elimination of the HIV prevention division within the CDC and cuts to funding for the nationwide Diabetes Prevention Program by the NIH.7
Medicaid expansion continued to be a critical tool for improving health outcomes, reducing uninsurance, and ensuring access to care for millions of low-income Americans.6 However, its future, especially in the Southern states that had not yet adopted it, remained subject to intense political debate and potential federal policy shifts.5,6 Although the American Rescue Plan Act of 2021 offered a temporary financial incentive—a 5 percentage point increase in the traditional Medicaid match rate for 2 years—that could more than offset state expansion costs, the temporary nature of this benefit and ongoing federal proposals for cuts created an uncertain outlook.10
References
1. Status of state Medicaid expansion decisions. KFF. August 26, 2025. Accessed August 29, 2025. https://www.kff.org/medicaid/issue-brief/status-of-state-medicaid-expansion-decisions/
2. Grossi G. 5 challenges the Affordable Care Act overcame in the last 15 years. AJMC®. April 25, 2025. Accessed May 20, 2025. https://www.ajmc.com/view/5-challenges-the-affordable-care-act-overcame-in-the-last-15-years
3. Mathers J, Tolbert J, Chidambaram P, Cervantes S. 5 key facts about Medicaid expansion. KFF. April 25, 2025. Accessed May 20, 2025. https://www.kff.org/medicaid/issue-brief/5-key-facts-about-medicaid-expansion/
4. Cervantes S, Bell C, Tolbert J, Damico A. How many uninsured are in the coverage gap and how many could be eligible if all states adopted the Medicaid expansion? KFF. February 25, 2025. Accessed August 29, 2025. https://www.kff.org/medicaid/issue-brief/how-many-uninsured-are-in-the-coverage-gap-and-how-many-could-be-eligible-if-all-states-adopted-the-medicaid-expansion/
5. Medicaid state fact sheets. KFF. May 20, 2025. Accessed August 29, 2025. https://www.kff.org/interactive/medicaid-state-fact-sheets/
6. Guth M, Ammula M. Building on the evidence base: studies on the effects of Medicaid expansion, February 2020 to March 2021. KFF. May 6, 2021. Accessed August 29, 2025. https://www.kff.org/affordable-care-act/report/building-on-the-evidence-base-studies-on-the-effects-of-medicaid-expansion-february-2020-to-march-2021/
7. Grossi G. Health policy in flux: Trump administration updates. AJMC. May 20, 2025. Accessed August 29, 2025. https://www.ajmc.com/view/health-policy-in-flux-trump-administration-updates
8. Shaw ML. Proposed GOP Medicaid cuts threaten loss of coverage for millions. AJMC. May 12, 2025. Accessed August 29, 2025. https://www.ajmc.com/view/proposed-gop-medicaid-cuts-threaten-loss-of-coverage-for-millions
9. Bonavitacola J. Supreme Court decision on Braidwood protects insurance coverage of preventive care. June 27, 2025. Updated June 27, 2025. Accessed August 29, 2025. https://www.ajmc.com/view/supreme-court-decision-on-braidwood-protects-insurance-coverage-of-preventive-care
10. Rudowitz R, Corallo B, Garfield R. New incentive for states to adopt the ACA Medicaid expansion: implications for state spending. KFF. March 17, 2021. Accessed August 29, 2025. https://www.kff.org/medicaid/issue-brief/new-incentive-for-states-to-adopt-the-aca-medicaid-expansion-implications-for-state-spending/
