- Center on Health Equity & Access
- Clinical
- Health Care Cost
- Health Care Delivery
- Insurance
- Policy
- Technology
- Value-Based Care
Contributor: COVID-19 Ranked Among the Top 5 Telehealth Diagnoses Nationally in April 2022
COVID-19 was ranked in the top 5 diagnoses through telehealth in the Midwest, Northeast, and West regions as well as nationally in the month of April, coinciding with an increase in COVID-19 cases.
In April 2022, COVID-19 returned to the top 5 telehealth diagnoses nationally for the first time since January, according to FAIR Health’s Monthly Telehealth Regional Tracker (FIGURE 1). COVID-19 also returned to the list of top 5 telehealth diagnoses in every US census region except the South; it had been off the list in all 4 regions (Midwest, Northeast, South, and West) since January.
The data represent the privately insured population, including Medicare Advantage and excluding Medicare fee-for-service and Medicaid. The reappearance of COVID-19 on the national and regional lists coincided with a rise in COVID-19 cases in April reported by the CDC.
FIGURE 1. Monthly Telehealth Regional Tracker, April 2022, United States
Credit: FAIR Health

Also in April 2022, telehealth utilization, as measured by telehealth’s share of all medical claim lines, grew nationally and in every region after 2 months of decline, according to the Monthly Telehealth Regional Tracker. National telehealth utilization increased 6.5%, from 4.6% of medical claim lines in March to 4.9% in April.
Regionally, the greatest increase was in the South, where telehealth utilization grew 11.8% in April. The rise in telehealth utilization may have been due to the growth in the reported number of COVID-19 cases, which may have led more patients to avoid in-person care.
Diagnoses
Various other diagnoses dropped off the lists as the share of COVID-19 diagnoses increased. Nationally, substance use disorders fell off the list; in the Midwest and Northeast, joint/soft tissue diseases and issues did so; and in the West, endocrine and metabolic disorders did so. In all regions and nationally, mental health conditions remained the top-ranking telehealth diagnosis.
Specialties
The rankings of the top 5 telehealth specialties did not change nationally or regionally in April 2022 when compared to March 2022, with social worker remaining the top-ranking telehealth specialty in all regions and nationally. But primary care physician increased its percentage share of telehealth claim lines by about 1% nationally and in the Northeast and South (FIGURE 2).
FIGURE 2. Monthly Telehealth Regional Tracker, April 2022, Northeast
Credit: FAIR Health
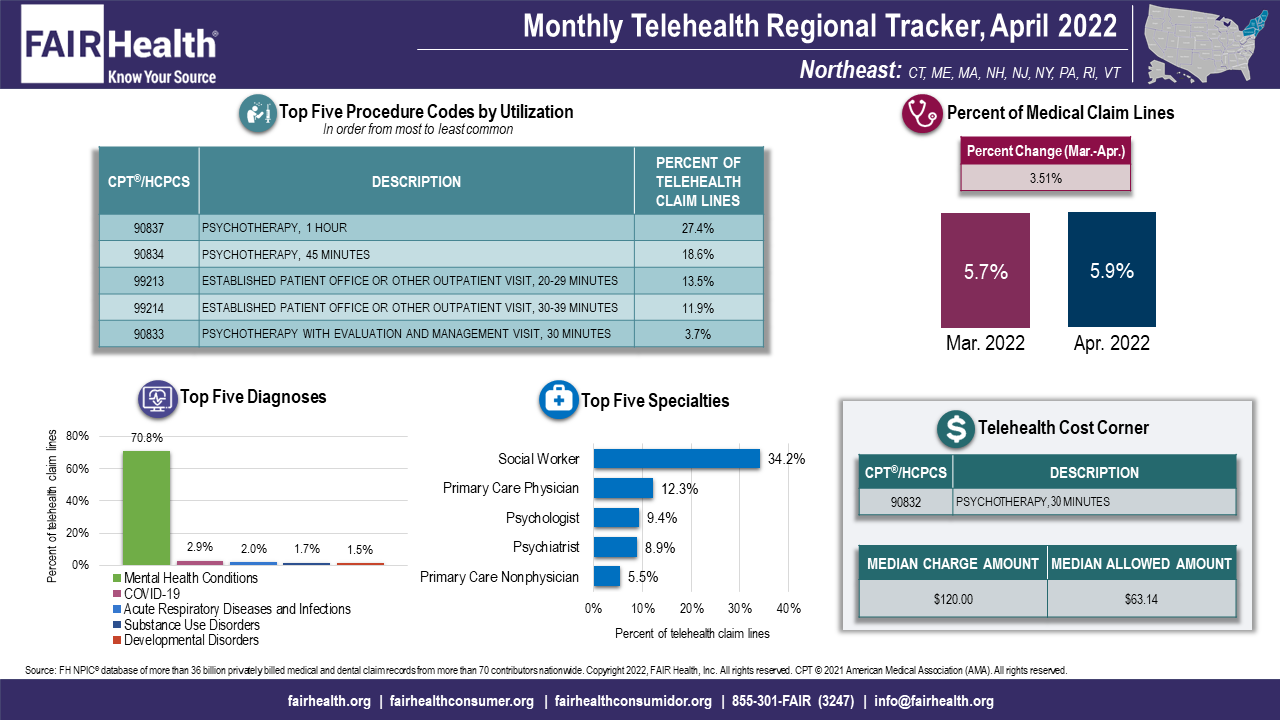
Procedure Codes
In April 2022, the rankings of the top 5 telehealth procedure codes did not change nationally or in any region when compared to the prior 2 months. The number 1 telehealth procedure code nationally and in every region remained CPT 90837, 1-hour psychotherapy.
Costs
For April 2022, the Telehealth Cost Corner spotlighted the cost of CPT 90832, 30-minute psychotherapy. Nationally, the median charge amount for this service when rendered via telehealth was $115.40, and the median allowed amount was $64.84.
About the Monthly Telehealth Regional Tracker
Launched in May 2020 as a free service, the Monthly Telehealth Regional Tracker uses FAIR Health data to track how telehealth is evolving from month to month. An interactive map of the 4 US census regions allows the user to view an infographic on telehealth in a specific month in the nation as a whole or in individual regions. Each infographic shows month-to-month changes in telehealth’s percentage of medical claim lines, as well as that month’s top 5 telehealth procedure codes, diagnoses, and specialties. Additionally, in the Telehealth Cost Corner, a specific telehealth procedure code is featured, with its median charge amount and median allowed amount.
